Volume 20 · Issue 2 ·March/April 2010 | Download PDF
by Séamus Kennedy, BEng (Mech), CPed
 The first rule of shoe selection for amputees is to consider the cause of amputation. If the amputation was the result of diabetes, then protecting the sound foot is of paramount importance
The first rule of shoe selection for amputees is to consider the cause of amputation. If the amputation was the result of diabetes, then protecting the sound foot is of paramount importance
Choosing the right shoe; what could be easier? Often, the decision depends more on your mood or your wallet than anything else. For amputees or people with complications from vascular disease, life is not so simple. Selecting the proper footwear may be an integral part of long-term health considerations, and this leads to more limited choices.
Diabetes
Uncontrolled diabetes and the resulting high blood sugar levels lead to nerve degeneration, or neuropathy. This loss of feeling usually starts at the extremities, in the hands and feet, so particular attention needs to be paid to any wounds or lesions that may begin to develop there. Because of the repetitive stresses and constant weight on the feet during walking, the foot is the main site for ulceration for patients with peripheral neuropathy. It is also difficult to heal these foot ulcers because most patients want to remain active and prefer not to sit around waiting for wounds to close.
Recognizing the importance of protecting these “at-risk” feet (and avoiding costly amputations), Congress enacted the Medicare Therapeutic Shoe Bill in 1993 to provide proper footwear and inserts for people with diabetes who qualify under Medicare Part B. The program was designed to prevent lower-limb ulcers and amputations in people who suffer from the disease. Eligible patients qualify for one pair of shoes, plus extra pairs of inserts and/or shoe modifications, for each calendar year.
These facts set the stage for many of the extra-depth and therapeutic shoes that are available on the market today. In response to the need for protective footwear, many pedorthic shoe manufacturers developed products with removable insoles, extra cushioning, seamless and stretchable uppers and wide supportive soles.
 Shoe Selection
Shoe Selection
The first rule of shoe selection for amputees is to consider the cause of amputation. If the amputation was the result of diabetes, then protecting the sound foot is of paramount importance. This is also true for people without diabetes if they have any similar symptoms such as nerve damage, poor circulation or a history of ulcers. In these situations, protection becomes the overriding concern.
Sometimes, despite the best of intentions and efforts, nothing can be done to prevent the advancement of wounds and ulcers. To limit further and far more serious complications, the best option, at times, is to amputate.
Certified pedorthists are trained to first look for the correct fit and function in a shoe, and only then do they consider cosmetics. Proper shoe fit begins with measuring foot size: both feet (if you are not an amputee) and each time you need a new pair. Swelling, weight gain and aging can all play a role in foot size and determining the appropriate shoe.
Good shoes are not too roomy or too tight. Big shoes will not hold the foot in place and they allow sliding inside, which potentially leads to “jamming” of the toes or shearing, which can irritate the skin. Conversely, shoes that are too small will reduce circulation or may cause blisters. In addition, good shoes will have firm counters (the stiffer portion at the back of the shoe) to help stabilize the heel and supportive soles that provide shock absorption. Sometimes the sole may be a little wider, or flared; this provides a broader base to control the motion of the foot as you walk.
When necessary, as determined by a medical professional, you may need a customized insole or a custom orthotic for the shoe. This will replace the removable inlay. Having a custom insole molded to the bottom of your foot will help even out the pressure and relieve points of irritation.
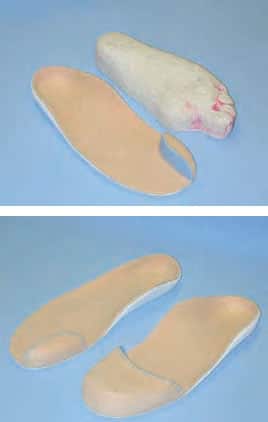
Partial-Foot Amputations and Toe Fillers
Sometimes, despite the best of intentions and efforts, nothing can be done to prevent the advancement of wounds and ulcers. To limit further and far more serious complications, the best option, at times, is to amputate. Though some amputations may require a prosthetic device, many foot amputations remove only a small part of the foot or a single toe.
These partial amputations do not require full prosthetic devices. However, patients can benefit from a toe filler that mimics and replaces the portion that has been removed. Good fillers may allow patients to continue wearing their existing wardrobe of footwear, and cosmetic acceptance can often be a big part of getting beyond the surgical loss. Without a toe filler, the foot may have too much room and slide inside the shoe; or the upper shoe may crumple or collapse at the site of the missing digit or digits. Toe fillers can be made from a variety of materials, such as foam or cork, and are often incorporated onto custom foot orthoses. They can then be moved from shoe to shoe.
Shoes for Prosthetic Feet
As previously stated, the No. 1 consideration for patients with a full prosthetic foot is to preserve and protect the remaining foot. If the “good” foot is in danger of breakdown, the patient needs to consider extra-depth shoes (as discussed above) or perhaps even a custom molded shoe. A custom molded shoe is made from a plaster cast of the patient’s foot. It is specifically designed and constructed with a custom insole to enclose the foot without any restrictions. Some patients are concerned with cosmetics, so custom shoes are often made for both the good foot and the prosthetic to provide a matching pair.
If the patient has a prosthetic foot, and there are no other health concerns for the good foot, it can still be difficult to get the right shoes. Sometimes, they have to consider buying two pairs of the same style shoes just to get the proper fit on each foot. Listed below are Web sites and services that help prosthetic wearers exchange single shoes to avoid these extra expenses:
oddshoefinder.com
oddshoe.org at 408/892-3484
Choosing the right shoes is an important aspect of overall health. Active patients feel better, respond better to treatment and tend to do better in the long run. Pedorthists have a passion for footwear, and they will be delighted to help patients find the right fit and function.
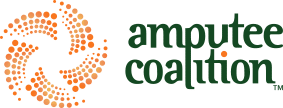


 Shoe Selection
Shoe Selection