Volume 15 · Issue 3 · May/June 2005
by Douglas G. Smith, MD

Oh, Those Unwanted Extra Pounds!
One major challenge with socket fit is weight gain, especially in the United States. This is especially true for people who were extremely active before their amputation. After the amputation, they tend to eat the same as before, but they’re no longer burning off as many calories as quickly. As a result, their weight increases, sometimes dramatically. Many adults who have very high lower-limb amputations gain weight, and any time you gain more than 10 to 15 pounds, your socket no longer fits correctly.
I remember a hard-working, broad shouldered, muscular construction worker who, while a little on the heavy side, would not have been considered fat. He lived a very active life, burning off a ton of calories every day at work and at play. But one day he was crushed in a cave-in at a construction site and lost a leg at the hip. Afterward, he was “down in the dumps.” He ate more than he was used to, drank a little bit too much, and, unfortunately, gained a heck of a lot of weight. He put on more than 80 pounds. As his weight went up, the soft tissue around his pelvis definitely expanded, and the prosthesis dug in more and more.
We made several major attempts to fit him with a comfortable prosthesis, but none of them worked well while he was sitting. “The prosthesis fits OK when I’m standing up and walking,” he told me,“but I just hate it when I’m sitting down.” So he never used it. Finally, he said, “I’ve mastered walking in this thing, but it just takes too much energy. I’m faster in my wheelchair or with crutches and a one legged gait. I spend a lot more time sitting than walking, and I really hate sitting in this socket.”
After learning to walk with the prosthesis, he made the informed decision that he’d prefer to go through life without it.
The one-legged, swing-through gait he referred to is very common for people with these high amputation levels. The person puts both crutches forward and places the tips against the ground, then swings his or her sound leg through until it touches the ground in front. He or she then loads the body’s weight onto the leg and repeats the motion. This gait style is often seen as a temporary transition until a person walks with a prosthesis, but, in reality, it’s probably the No. 1 form of ambulation used full time by people with these high amputation levels.
Realizing the importance of emphasizing a healthful diet and the risk of weight gain, we now counsel people early on to try to prevent them from putting on extra pounds because prevention is not nearly as difficult as losing the weight after it’s put on. Typically, this is not something people want to deal with in the first weeks following amputation, but it’s important. The healthcare team has to be aware that this person has a real potential for unwanted weight gain with serious consequences.
We also need to realize that weight gain and weight loss aren’t the only factors that affect the fit of a prosthesis. How often the person uses his or her prosthesis also plays a part. People can use their prosthesis full time, part time, sporadically, or not at all. Full-time users put on their prosthesis when they get up in the morning and use it until they go to bed at night. Part-time users typically select specific times and activities for wearing their prosthesis. They might, for example, wear their prosthesis three times a week for a specific reason, such as going shopping. Sporadic users may have trouble maintaining the fit of their prosthesis, even without gaining or losing a bit of weight. They might, for example, decide to wear their prosthesis just a couple of times a month. For the first month or two, there may be no problems. By the third month, however, it doesn’t fit anymore. What happened? Basically, if you don’t use your prosthesis full time or semi-regularly, the soft tissues near the amputation site can change subtly but have a big impact on socket fit. By wearing the prosthesis on a regular basis, you get used to the prosthesis, and the prosthesis helps maintain a consistent shape at the amputation site. It works both ways.
If It’s So Difficult, Why Try a Prosthesis at All?
Most laypeople think of prosthesis use only as a full-time phenomenon, and for some lower-limb amputees, it is. But with high amputation levels, the concept of part-time use often emerges (i.e., “I’m going to use it when I go out to the bridge club. I’m choosing when to use it. But I’m not going to wear it for the rest of the day because it’s just too heavy, and it digs in. I’m choosing not to use it later.”) There are times when people want to be standing up and walking. At other times, it’s not necessary or just not comfortable to do so.

Since many people with these highlevel amputations eventually decide not to use their prosthesis, you might ask,“Then why go through the struggle – and the expense – of getting a prosthetic leg and learning to use it?”
For the most part, I’ve found that people want very much to try to master using a prosthesis. Those who are never given a chance often feel cheated. They can become frustrated and very bitter. People see others who have learned to use a prosthesis, and many of them ask, “Why not me?” If they’re not given a chance, they may even feel betrayed or that healthcare professionals have given up on them. While it certainly is disappointing to struggle to learn to use something and then to decide it’s just not going to work for you, my patients tell me that it would be far worse to never be given a chance to try.
So, many give prosthetics a go. Generally, a group of them succeed in using a prosthesis full time. Others use it on a part-time basis or sporadically, and some then make the choice that a prosthesis is just not for them. We typically see the decision-maker whose job includes approval or denial of a prosthesis as a cold-hearted miser sitting behind a big, imposing desk. Actually, that man or woman represents society and all of the people who pay insurance premiums or taxes to the government. If that person is careless on the job, insurance premiums or taxes have to go up. The decision can affect many people. So why should society pay for a prosthesis that two out of three people end up not using? Isn’t there a better way to pick who’s going to be successful?
Unfortunately, there’s not one we know of yet. There simply is no magic crystal ball. I strongly believe that if a person first masters the vital skills and still wants to get a prosthesis, then he or she deserves a chance. It may be used full time, part time, sporadically, or, ultimately, not at all, but in any scenario, the person deserves a chance to try.
Many need to prove to themselves that they “can” use a prosthesis and then to decide whether they really “want” to use one. Then, it isn’t a matter of not using it because you don’t know how or aren’t good enough. Rather, you’ve made a choice, like the construction worker mentioned earlier, and can say, “I’ve mastered it. I can do it. Now, I’m going to decide if I really want to use it.”
How About a Wheelchair?
Some people, whether they choose to use a prosthesis or not, opt to use a wheelchair some or all of the time. Most hip- and pelvic-level amputees see it as an additional necessity for getting around, especially if they don’t feel safe using their prosthesis on a particular day because of fatigue, soreness, or other factors. Others tell me that they find a wheelchair simpler than a prosthesis and that they get around faster in one.
But wheelchair users certainly face barriers. For starters, the world just isn’t made for wheelchairs. Between stairs, inclines, curbs, uneven surfaces, narrow passages, and tight spaces, it can be challenging to get around. In addition, routine maintenance and upkeep are required to ensure that the chair is kept in good working order. Though there are a wide variety of chair types available, ranging from the simple, stripped down ones to the fully loaded, sometimes complex, models, I think it’s worth noting that sometimes less can actually mean more. It’s easy to be dazzled by all of the technological advances. You tell yourself, “Hey, I might need those,” and end up buying a chair with many features that you will rarely, if ever, use. Certainly, we’re glad that people who need or want all those chair functions have them at their disposal. But, interestingly, people who have used wheelchairs on a long-term basis typically come to prefer those chairs that are simplest in appearance and function. There aren’t a lot of “bells and whistles.” The person wants a chair that’s light, easy to maneuver and low-maintenance. Through experience, people often find that a lot of gadgets can end up being more trouble than they’re worth. The fewer moving parts there are, the lower the chance of something wearing out or breaking.
Innovation
Seating assessments must be made to best accommodate each individual. Although there are many seating systems that can provide both support and comfort, we also need to keep in mind that sitting without the prosthesis is very different from sitting with it and try to make sure that each person is accommodated accordingly.
One of the most innovative concepts I’ve seen involved a young man who had a transpelvic amputation as the result of an explosion. He took the blast from the side, and after surgery, he was left with a transpelvic amputation site with scars, fragile skin grafts and very little padding. It was a major challenge for him to sit without pain or tissue breakdown.
Early in the young man’s rehabilitation, one of our therapists designed a pair of bicycle shorts for him that were of normal thickness on one side and had a thicker, custom-molded gel pad sewn into the amputated side. That gel cushion really redistributed the forces he felt when sitting. The leg hole on the amputated side was sewn shut to give him a better fit. Every morning, he’d put on his underwear, then his customized bicycle shorts, and finally his regular pants. He found that the shorts were beneficial for both sitting in his wheelchair and when he moved to other seating surfaces. They had built-in support that he took with him wherever he went. Before he had his personally designed shorts, he would tip to the amputated side whenever he sat. The shorts gave him added cushion that helped level his back so he could sit comfortably. Also, he and his girlfriend told me that they liked the way his“personalized” shorts gave his backside a better appearance.
I’ve always thought that those shorts were a creative solution to the problems and should be used more often. When most people think of seating systems, they tend to focus on a cushion that goes into a wheelchair or a cushion that you can take with you and use from chair to chair. But the young man with the bicycle shorts told me that he hated having to carry that cushion with him everywhere; the bicycle shorts not only clothed him, but they also gave him a seating system he could wear.
Functional Scoliosis
Most of us have heard of scoliosis, or curvature of the spine. There are two major forms of scoliosis. One kind is anatomic and fixed. You can be born with it or it can occur as you grow. It can also result from a traumatic injury. Anatomic and fixed scoliosis means there’s a real curve to your spine that’s there all of the time.
The other kind of scoliosis is functional and postural. It is totally dependent on positioning. When you’re lying down at rest, the spine can be perfectly straight. But the lower spine may curve dramatically while you’re sitting or standing. Though functional and postural scoliosis is seen in many upper- and lower-limb amputees, it can be very dramatic after a pelvic-level amputation, especially when sitting. This occurs, in part, because sitting while wearing the socket causes the amputated side to lift up higher than the other side so that the person no longer is sitting levelly. Standing may also cause the spine to curve because the prosthetic leg is typically just a bit shorter than the nonamputated leg.
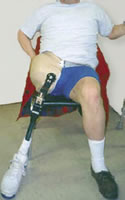
Sitting with a hip-level prosthesis can tip the pelvis up and cause functional scoliosis. The prosthesis can also dig uncomfortably into the groin and abdominal areas. Sockets made with softer, more flexible material can help but still do not eliminate these problems.
Sitting in the prosthesis can push up the pelvis on the amputated side. Without the prosthesis, sitting can cause that side to tip down because of the loss of soft tissue. To get an idea of what this is like, sit with a book under one buttock. Do you feel how your pelvis tips and your head drifts over to one side? To get your head back up over the center of your body, you have to sit with a postural curve in your lower spine. This is the kind of scoliosis that can affect people with high-level amputations. When they sit with their prosthesis, they must curve their spine one way; when they sit without it, they must curve their spine the other way.
Not surprisingly, a person with functional scoliosis is likely to experience some back pain as a result of added wear and tear on the spine. One way to deal with this is with a pelvic leveler. This is usually a special cushion with padding positioned so that the pelvis is level when the person sits. Our friend with the special bicycle shorts had, in effect, a built-in pelvic leveler. He needed the additional padding on his amputated side so that he could sit levelly. But, interestingly, some hip-level amputees, when wearing their prosthesis, will need the additional padding on the nonamputated side because the bulkiness of the prosthesis lifts the amputated side higher.
While back pain is a widespread problem among people in general, those with amputations have a higher incidence of back pain. In one survey, lower-limb amputees listed back pain as a more bothersome problem than phantom pain. Yes, there are many causes of back pain, but gait deviations following amputation and uneven sitting contribute to the problem. For some, a pelvic leveler can help.
Energy and Our Emotional Selves
As we’ve looked at the challenges in adjusting to life after a hip disarticulation or transpelvic amputation, what emerges is that it takes a great deal of energy to re-learn to walk. For some, it’s an exhausting process. Most people believe that it can take more energy to get from one point to another using a hip-level prosthesis than it does with a one-legged gait and crutches. Besides that, it generally takes even less energy to use a wheelchair. Balance problems and fear of falling are additional reasons that many people with these amputations use prosthetic limbs for only short amounts of time or not at all.
In addition to the physical changes and challenges brought about by these amputations, there are strong emotional factors involved. In fact, for many people, the emotional issues matter most. It’s worth noting that the emotional intensity does not always match the level of the amputation. I’ve seen a few people whose lives are totally derailed by the loss of a toe, while others who have lost a leg and part of their pelvis hardly miss a beat.
But, in general, there seem to be more emotional and complex issues with these high amputation levels, such as increased difficulty with prosthetics, difficulty “blending in with the crowd,” and more dramatic changes in gait and ambulation. Also, as we discussed earlier, there may be possible changes in bowel, bladder and sexual functions and issues with an amputation that approaches the core of the body.
Folks with these amputation levels often tell me that they don’t feel totally included in support groups. The tendency in support groups is to talk about walking and prosthetics, and that’s quite normal for transtibial and transfemoral amputees. But people with these lower-level amputations frequently don’t understand the complexity and challenges of amputations in the hip and pelvic areas. They may unwittingly make people with higher-level amputations feel less than successful by suggesting that the best way to measure success is by walking. Walking and transfer issues certainly are important for all lower-limb amputees, but other challenges may not be addressed or understood by those support group members who have not experienced them.
What Is Success?
How do we measure success? With most lower-limb amputations, people automatically define success as walking again. But with hip disarticulations or transpelvic amputations, we definitely can shortchange a person’s accomplishments if our only marker of success is walking. For people with these high amputation levels, success is, first and foremost, surviving. Then we can measure success by transfers, getting on and off of the toilet, and mastering the basic skills. Success is re-creating mobility and independence, first with a wheelchair, then with a walker, then with a one-legged gait with crutches, and, ultimately for some, with a prosthesis. If your goals are sequential, you can’t define success only by reaching the last step. As actress Helen Hayes said, “Always aim for achievement, and forget about success.”
People with these high amputation levels can be made to feel “unsuccessful” if they don’t walk again, and it shouldn’t be that way. Comments by family, friends, therapists or physicians that are meant to be encouraging can, instead, be devastating. They don’t realize the complex decisions that are made every day by a person with a hip- or pelviclevel amputation. A comment that’s meant to be encouraging– “We’re going to get you walking with your prosthesis!”– can haunt a person who is thinking that perhaps crutches or a wheelchair would be preferable. A comment about walking may be interpreted as, “You’re not walking. You’re a failure.”
We have to learn to take pride in each success along the way and know when to say when. Someone who is pushing you harder and harder to be successful may have good intentions but might not really understand and appreciate what you’ve already accomplished. This can ruin any future interactions. Comments that are meant to be encouraging and well-meaning can instead have a big detrimental effect– and the person saying them may not even realize it! More beneficial, perhaps, would be good questions: “What are your goals?” “What do you want?” “Are you satisfied?”
In measuring success, we have to look at what each individual accomplishes. A person shouldn’t be made to feel bad because he or she doesn’t master walking or masters it but chooses not to do it. President Lincoln once said, “I am a slow walker, but I never walk backwards.” This comment illustrates that moving fast may not count as much as moving ahead. Progress is progress, regardless of speed and the way we move. Progress is what most of us want. Each of us needs to find the best way to get it.