Volume 14 · Issue 2 · March/April 2004 | Download PDF
by Douglas G. Smith, MD, Amputee Coalition Medical Director

Though the transfemoral amputation can be a challenging amputation level for the amputee, the surgeon, prosthetists, therapists, and every member of the healthcare team, it is still required fairly often, despite the tremendous emphasis in recent decades on preserving amputation levels in the foot and below the knee.
Still, more transfemoral amputations are required than many people realize. Of the more than 1.2 million people in the United States living with limb loss, 18.5 percent are transfemoral amputees, according to the latest figures provided by the National Center for Health Statistics. A study by Dr. Timothy R. Dillingham and colleagues titled Limb Amputation and Limb Deficiency: Epidemiology and Recent Trends in the United States, which was published in theSouthern Medical Journal (2002), offers more statistics. The study, provided to us by the National Limb Loss Information Center (NLLIC), shows that there were 266,465 transfemoral amputations performed in the United States from 1988 through 1996 (the most recent years available). That’s an average of 29,607 annually. Statistically, almost one of every five people living with limb loss in this country has a transfemoral amputation.
In the United States, this amputation level is most commonly known as an above-knee amputation, or AK. Internationally, it’s referred to as a transfemoral amputation because the amputation occurs in the thigh, through the femoral bone (femur). Today, the international terminology is gaining favor as a more definitive description of the amputation level involved. Plus, using international nomenclature puts us more in line with the rest of the world.
While the transfemoral amputation level is fairly common, there’s nothing simple about adjusting to life after surgery. The person living with transfemoral limb loss faces distinct challenges, such as increased energy requirements, balance and stability problems, the need for a more complicated prosthetic device, difficulty rising from a seated position, and, unlike with amputation levels in the tibia and the foot, prosthetic comfort while sitting.
Energy and Speed
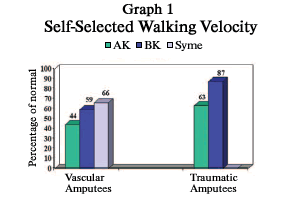
A study by Dr. Robert L. Waters and co-workers titledEnergy Cost of Walking of Amputees: The Influence of Level of Amputation, which was published in The Journal of Bone and Joint Surgery (1976), looked at gait and energy use among 70 people with lower-limb amputations. Transfemoral, transtibial and Syme amputations resulting from vascular disease and trauma were compared among the participants with limb loss and to a control group of individuals without amputations. As Graph 1 illustrates, the chosen velocity of walking for vascular amputees was 66 percent of that for nonamputees at the Syme level, 59 percent at the transtibial level and 44 percent at the transfemoral level. Among trauma amputees, velocity was 87 percent for the transtibial level and 63 percent for the transfemoral level. In short, the higher the amputation level, the slower the walking speed. Trauma amputees walked faster than vascular amputees primarily because of age differences and overall health status. By the time blood vessels in the legs are diseased to the point where amputation is needed, individuals with vascular disease also have significant disease of the blood vessels in the heart and lungs. Gait improved and the energy required for prosthetic walking significantly decreased as amputation levels moved toward the foot.
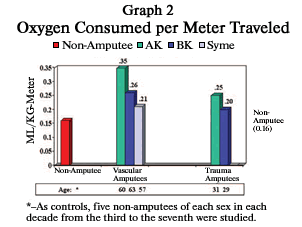
To measure energy, subjects are outfitted with a mask and a backpack containing an oxygen tank. As the person breathes in and out, sensitive monitoring equipment measures the amount of oxygen being inhaled and exhaled through the mask over a set distance. This oxygen use is then converted to the amount of energy that’s required to cover that distance. If your energy requirements increase, you breathe faster and use more oxygen. Graph 2 shows that the higher the amputation level, the more energy expended per meter traveled.
It’s not uncommon to slow down to the point where your energy use per minute approximates normal, but your energy use per distance walked – whether it is measured per meter, per 10 yards or per mile – increases substantially. But you may not feel fatigued because you’re burning that energy over a longer period of time.
A person with a transfemoral amputation usually walks more slowly than before but expends more energy over a longer time because it takes a greater effort to walk with an amputation in the thigh. To illustrate this, think of how you feel when you run a short distance as fast as you can and when you walk the same distance. Sprinting 100 yards will likely leave you out of breath, while walking will take you longer but will not leave you winded. A person with a transfemoral amputation walking 100 yards will, of course, take longer to cover that distance. But he or she will need to expend more energy to go that distance than does a person with a lower amputation level or no amputation. The factor that leaves you out of breath isn’t the total energy you expend; it’s how fast you expend it.
Another factor to consider is how energy expenditure will leave you feeling by the end of the day. We generally recover quickly from short, fast bursts of energy use and go about the rest of the day without feeling unusually tired. But if you walk more slowly for several hours, you’ll probably feel quite tired at the end of the day. You’ve expended less energy per second, but you’ve expended more energy over a longer period of time. For a person with a transfemoral amputation, it takes more energy to walk, even though he or she isn’t using as much energy per second.
Steps, Stairs and Other Ups & Downs
Inclines and stairs also become more challenging. Most people with transfemoral limb loss do not go “step over step” as they walk up or down stairs. Rather, they tend to go step by step, one stair at a time. Typically, an individual with transfemoral limb loss will first step up with the sound leg, then bring the prosthetic side up to the same step. This is because the prosthetic knee does not provide the power necessary to take the person up to the next higher step. The prosthetic knee would buckle as body weight was transferred to it in pushing up to the next stair, and the person would collapse. Newer, more advanced prostheses, such as the microprocessorcontrolled C-Leg, do allow some people to walk step over step, especially going down stairs. This is because it’s designed not to collapse. But even the most advanced, currently available knee units do not have a motor that provides lifting power.
Loss of knee power is one of the factors that make it very challenging to adjust to a new way of walking after a transfemoral amputation. The knee is an amazingly strong joint, and its power is vital for walking, rising, going from sitting to standing and vice versa, and transfers, such as getting in and out of the bathtub or on and off the toilet. After a transfemoral amputation, the muscles around the hip still move the thigh forward and back, but the prosthetic knee, contrary to a common misconception, cannot actively extend the lower leg out straight or bend it back into flexion. Prosthetic knee units are not run by muscles so they function, in a sense, like well-controlled passive hinges. Even with technological advancements, a prosthetic knee that can provide motor activity to take a person from standing to sitting the way a real knee does has not yet been made.
It Ain’t Easy
With all of these factors in mind, it’s no wonder that a patient of mine who had a transtibial amputation that was later, because of infection, revised to a transfemoral amputation, told me, “Doc, it’s not twice as difficult going from a BK (below-knee amputation) to an AK (above-knee amputation), it’s 10 times more difficult!” The biggest factor is the missing knee joint. He had to go from a prosthesis that essentially replaced one joint – the ankle – to one that replaced two – the ankle and the knee.

- Mental Energy: This refers to the conscious effort of thinking about walking, concentrating and moving with a prosthesis.
- The Stumble: This happens while walking or moving when the rhythm of the walk or movement is suddenly stopped or changed. A stumble does not mean actually falling down; instead, it can be thought of as a “near miss.” Recovery from a stumble often happens with a “stutter step,” a hop or a shift in weight balance.
- The Semi-Controlled Fall: This occurs when you lose your balance and start to fall. You recognize the fall as it is occurring and brace for it or grab onto something to either break the fall or help you land in a protected fashion. The semi-controlled fall may evoke feelings of embarrassment or frustration.
- The Uncontrolled Fall: This occurs during a sudden loss of balance when there’s insufficient time to protect yourself from the impact of the fall. This type of fall is more likely to produce injury and can make you feel angry, anxious and confused.
While stumbling and falling clearly are issues for all lowerlimb amputees, the higher the amputation level is above the knee, the greater the risks of falling. Walking is automatic for most individuals, with almost no conscious thought. A person with a transfemoral amputation, on the other hand, must really focus on walking, especially on uneven surfaces, stairs and inclines, and in unfamiliar areas. Different environments can bring different and sometimes hazardous challenges. It’s one thing to take a leisurely walk on an even, smooth pathway. It’s something else altogether to navigate an area such as an airport concourse where people are walking at many speeds, stopping and starting, and coming in and out of “your space” from all directions. You have to make countless adjustments to your gait as you walk to or from your gate.
I continue to be impressed by the number of people with this amputation level who master the skills needed to walk confidently with a transfemoral prosthesis. It’s a credit to the human spirit of perseverance that they’re able to face the many challenges brought by the loss of knee power and overcome them.
“Success consists of getting up just one more time than you fall.” – Oliver Goldsmith, Irish playwright